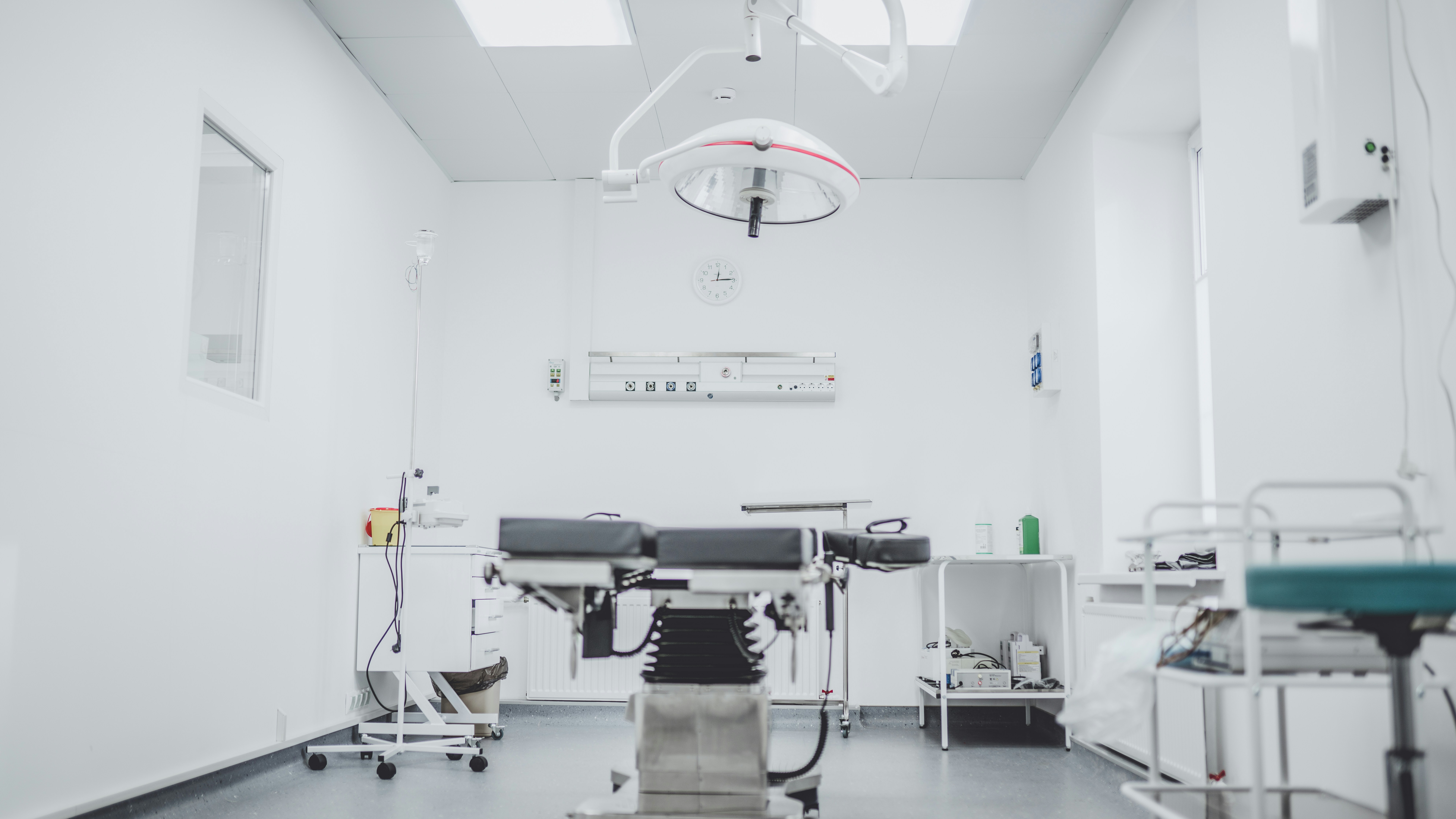
So, what does a surgical technologist do, hour by hour, phase by phase? More than most people expect – and the scope of the role goes far beyond the popular image of someone simply passing tools to a surgeon.
What Is a Surgical Technologist?
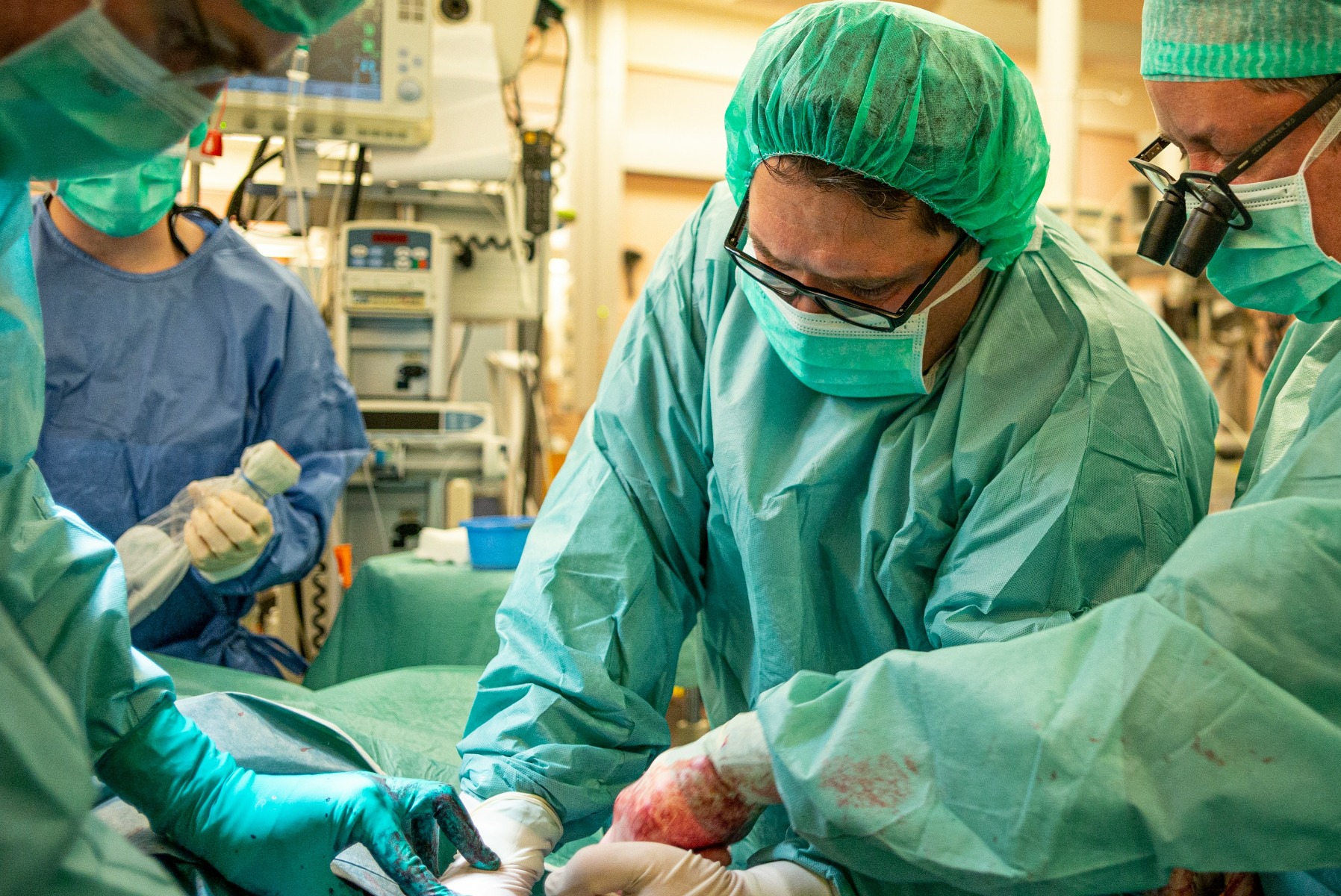
A surgical technologist – also called a scrub tech or OR technician – is an allied health professional who works directly within the sterile surgical field. They are not surgical nurses, and they are not physician assistants (PAs). They occupy their own lane: technically precise, procedure-focused, and deeply embedded in the mechanics of how a surgery unfolds.
"Surgical technologists are integral members of the surgical team, working under the supervision of surgeons and in collaboration with OR nurses and the anesthesia team. They play a critical role in patient safety by contributing to successful outcomes through precision, vigilance, and collaboration."
– Robin Y Jenkins, CAE, ICE-CCP, CEO of the National Board of Surgical Technology and Surgical Assisting (NBSTSA)
The profession has roots in World War II military medicine, when trained medics assisted surgeons on the battlefield. The job was built from urgency and precision, and those qualities never left.
As of 2024, the field employs about 115,600 surgical technologists across the United States, with the median annual wage landing at $62,830. Employment is projected to grow 5 percent from 2024 to 2034, faster than the national average for all occupations, with approximately 8,700 openings expected each year over that decade.
This is a field with staying power – driven by an aging population, advances in surgical technology, and the expanding footprint of outpatient surgery centers.
Pre-Operative Responsibilities: Everything Before the First Incision
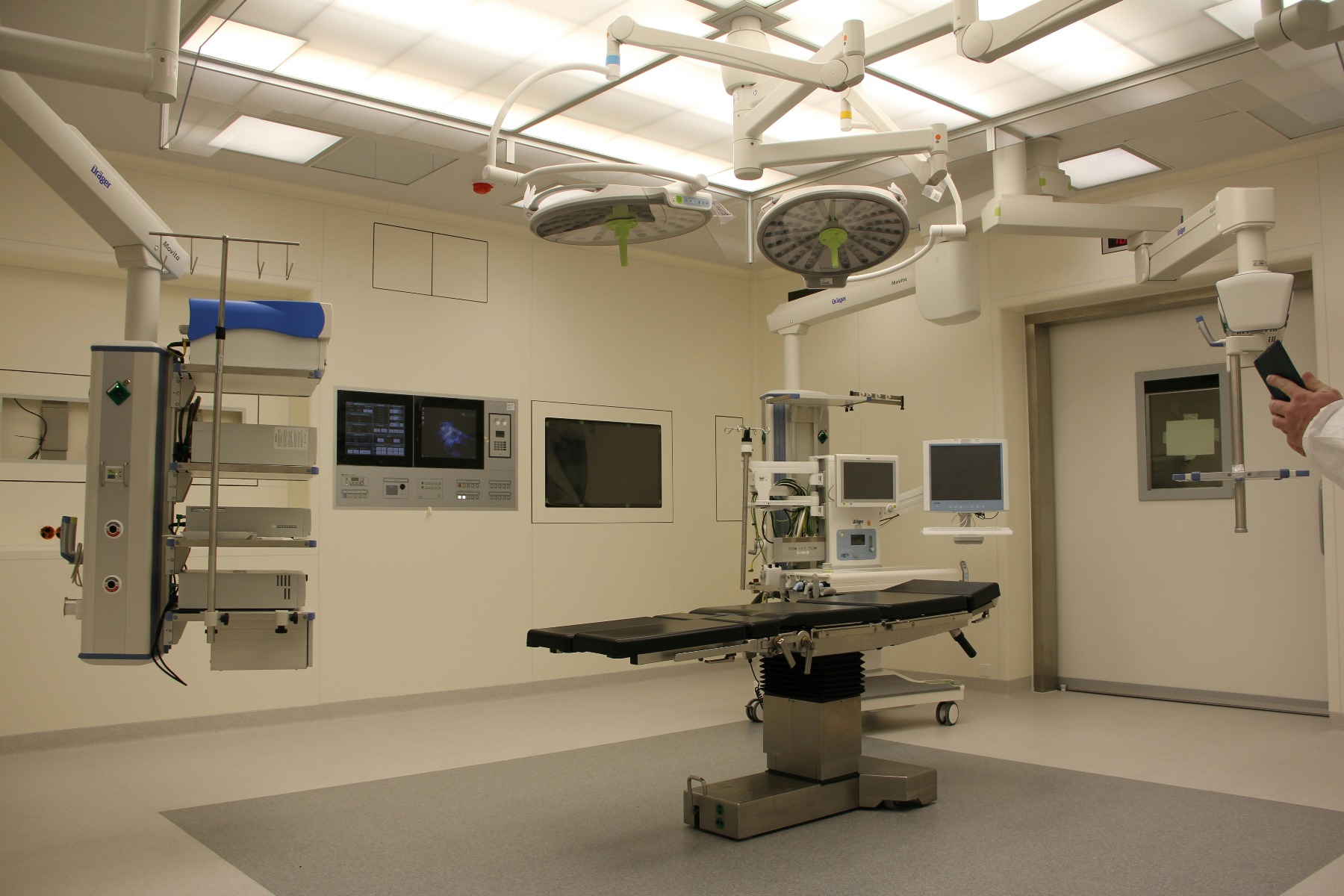
Most people assume surgery begins when the surgeon picks up a scalpel. It doesn't. By the time a patient is wheeled into the OR, a surgical technologist has already been there for an hour or more.
The pre-operative (pre-op) phase is where the groundwork is laid.
- Room setup and instrument preparation: The surgical tech reviews the scheduled procedure, identifies the specific instruments and supplies required, and sets up the sterile back table and Mayo stand (a smaller tray positioned directly over the patient during surgery). Every item on that table must be sterile, correctly placed, and arranged in the order the surgeon will need it.
- Instrument counts: Before any procedure begins, surgical technologists count all instruments and supplies with an operating room registered nurse – a step designed to protect patients from the retained foreign objects that can cause catastrophic post-surgical complications. This count happens three times: before surgery begins, before closure starts, and at the end of the procedure. A discrepancy triggers an immediate halt. The count includes sponges, needles, and even blade pieces. A retained sponge is one of the most common surgical errors in operating rooms worldwide – and the tech's count is a frontline defense against it.
- Patient preparation: The surgical tech helps transfer the patient onto the OR table, positions them correctly for the procedure type, and drapes them with sterile surgical coverings that define and protect the sterile field. They may also prep incision sites.
- Equipment checks: Surgical lights, suction machines, electrosurgical units, and specialized equipment – from laparoscopic towers to robotic surgical systems – all need to be operational before the first cut. Catching a malfunction pre-op is inconvenient. Catching it mid-procedure can be dangerous.
Intra-Operative Responsibilities: Working in the Sterile Field
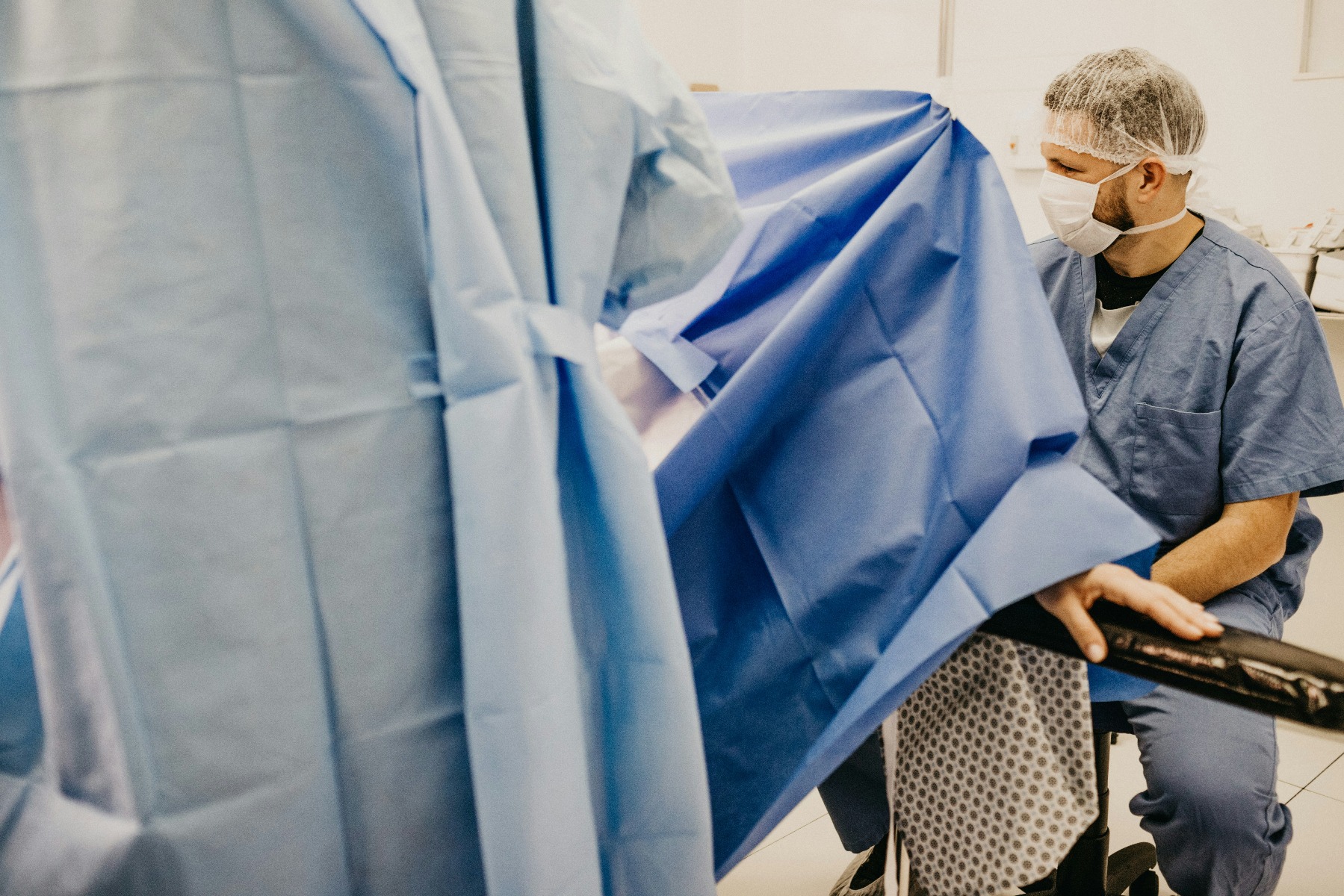
Once the procedure begins, the surgical technologist shifts into what the profession calls the "scrub role" – they are scrubbed in, gowned, gloved, and working inside the sterile field alongside the surgeon.
This is where the role becomes something closer to a high-stakes collaboration.
- Instrument passing: The tech anticipates what the surgeon needs before they ask for it. Handing the wrong instrument, or hesitating when milliseconds matter, creates friction in the OR. An experienced tech reads the procedure – they know a suture is coming next because they understand the anatomy of what's happening on the table.
- Maintaining the sterile field: Every touch, every movement inside the OR is governed by aseptic technique. The surgical tech is the primary guardian of sterile field integrity. If a glove tears, if an instrument brushes a non-sterile surface, if a team member reaches across the field incorrectly, the tech calls it. This is what the Association of Surgical Technologists (AST) refers to as "surgical conscience." It is a professional obligation to self-correct and to correct others, even in the middle of a procedure.
- Specimen handling: Tissue removed during surgery, such as biopsies, excised masses, and lymph nodes, must be handled correctly, labeled accurately, and prepared for pathology. A mislabeled or contaminated specimen can delay or derail a diagnosis.
- Equipment operation: Depending on the procedure, the tech may operate retractors to hold tissues in position, manage suction, assist with hemostasis (controlling bleeding), or interface with robotic surgical platforms like the da Vinci system.
- Counts (again): Instrument, sponge, and needle counts continue throughout the procedure, particularly before any body cavity is closed. The consequence of skipping this step is a patient going home with a surgical instrument sutured inside them.
If the scope of this role surprises you, that's the point. Surgical technology is a skilled, in-demand profession.
Health Tech Academy's online 16-week Surgical Technologist Certification Program gives you the foundational knowledge to step into this field with confidence.
The program leads to the National Registry Surgical Technologist (NRST) credential through the American Allied Health (AAH).
Get Certified in 16 Weeks →Hear from One of Our Students
Hear from Your Surgical Tech Instructor
Compare Health Tech Academy Vs Community Colleges Vs Online Colleges
| Metric | Health Tech Academy | Community College | Online Colleges |
|---|---|---|---|
| Program & tuition cost | $3,450 | $2,000 – $10,000/year | $8,000 – $19,000/year |
| Books, materials, & fees | Included ✓ | + $500 – $2,000 | + $500 – $2,000 |
| Certification exams & fees | Included ✓ | + $200 – $500 | + $200 – $500 |
| Job ready timeline | 4 – 6 months | 1 – 2 years | 6 months – 2 years |
| 100% online | ✓ Yes | ✗ No | ✓ Yes |
| Schedule flexibility | ✓ Yes | ✗ No | ✓ Yes |
| 1-on-1 coaching & mentorship | ✓ Yes | ✗ No | ✗ No |
| Job placement assistance | ✓ Yes | ✗ No | ✗ No |
| Clear path to certification | ✓ Yes | ✗ No | ✗ No |
| No travel requirements | ✓ Yes | ✗ No | ✓ Yes |
Post-Operative Responsibilities: After the Surgeon Steps Back
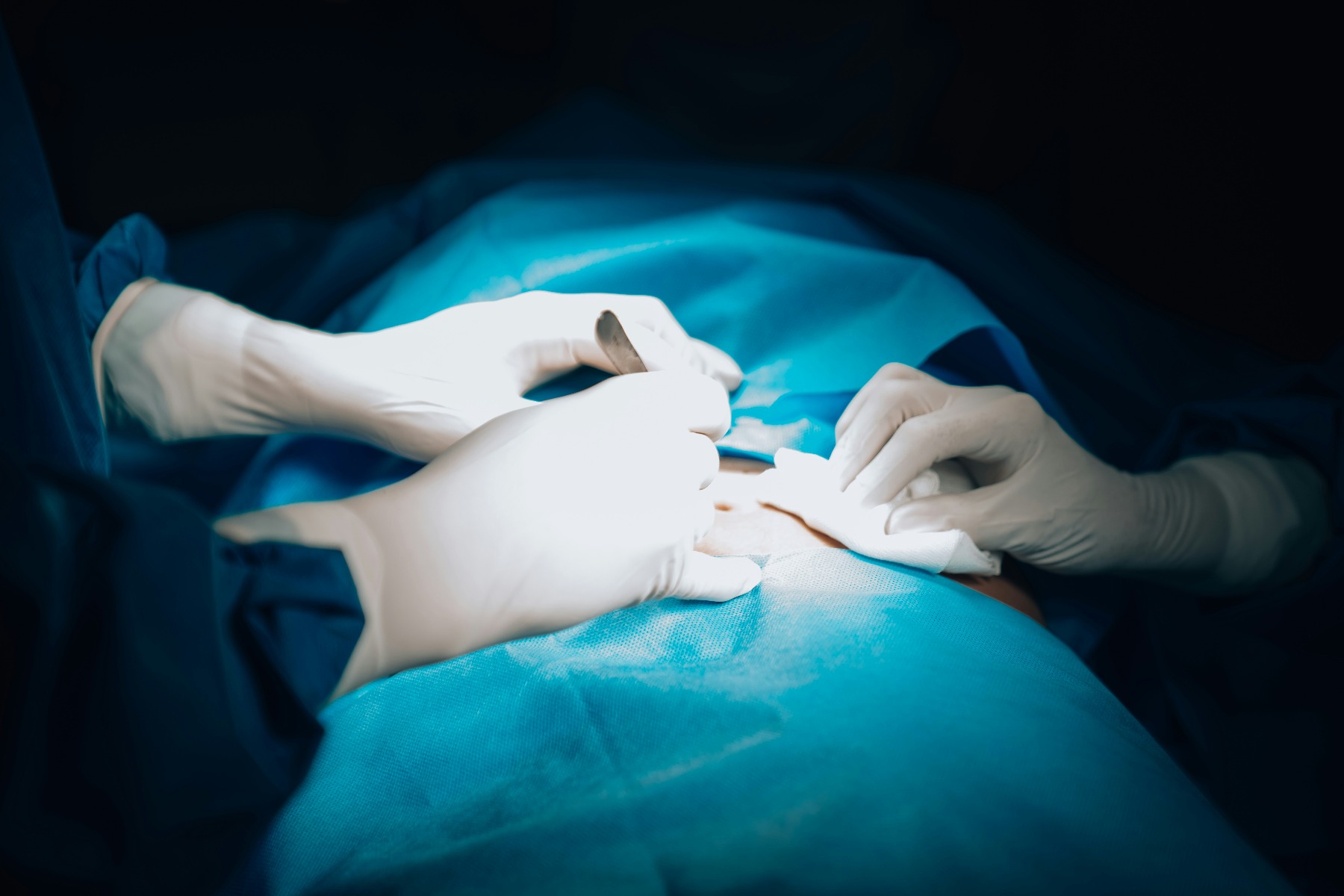
The procedure ends, but the surgical technologist's shift doesn't.
- Final counts and documentation: Every item counted at the start must be accounted for at the close. The tech and the circulating nurse conduct a final tally, and discrepancies are documented and investigated before the patient leaves the OR.
- Wound care: In some settings, surgical techs assist with applying sterile dressings to incision sites.
- Room breakdown: Used instruments are collected, decontaminated, and sent for sterilization. Disposable items are discarded following appropriate biohazard protocols. The room is cleaned and restocked in preparation for the next case.
- Patient transport: The tech may accompany the patient to the recovery area, where they provide a handoff report to post-anesthesia care staff.
What's worth noting: A busy surgical tech working in a hospital setting might turn over multiple OR rooms in a single shift, repeating this entire cycle back-to-back. The pace is relentless, and the margin for error throughout is essentially zero.
Skills and Tools of the Surgical Tech Trade

The OR is not a place where you learn on the job by watching. Surgical technologists arrive prepared.
Technical skills developed in training:
- Sterile and aseptic technique.
- Surgical anatomy and physiology.
- Instrumentation – knowing hundreds of instruments by sight, function, and name.
- Suturing and wound closure assistance.
- Pharmacology basics, including medications commonly administered during procedures.
- Robotic and laparoscopic equipment operation.
- Emergency response protocols, including cardiopulmonary resuscitation (CPR) and basic life support (BLS) techniques.
Instruments they work with daily:
- Scalpels.
- Retractors.
- Hemostatic clamps.
- Needle drivers.
- Electrosurgical units.
- Laparoscopic trocars.
- Irrigation systems.
- Surgical drills and saws (in orthopedics).
- Robotic instrument arms.
- An extensive variety of sutures and stapling devices.
Soft skills that determine who thrives:
- Anticipation – reading a surgical field well enough to know what comes next.
- Composure under pressure.
- Precision without being slow.
- Communication that is direct and free of ambiguity.
- Surgical technologists must possess manual dexterity, critical thinking, strong interpersonal skills, and the emotional stability to handle the demands of the operating room environment.
Surgical techs are often the most specialized people in the room in terms of procedural knowledge. While a surgeon may focus on performing a procedure, the tech's entire training is built around supporting that procedure from the sterile side. They study specific surgical specialties – orthopedics, neurosurgery, cardiovascular surgery, and ophthalmology – and develop expertise that is deep.
How Training Prepares You for OR Settings
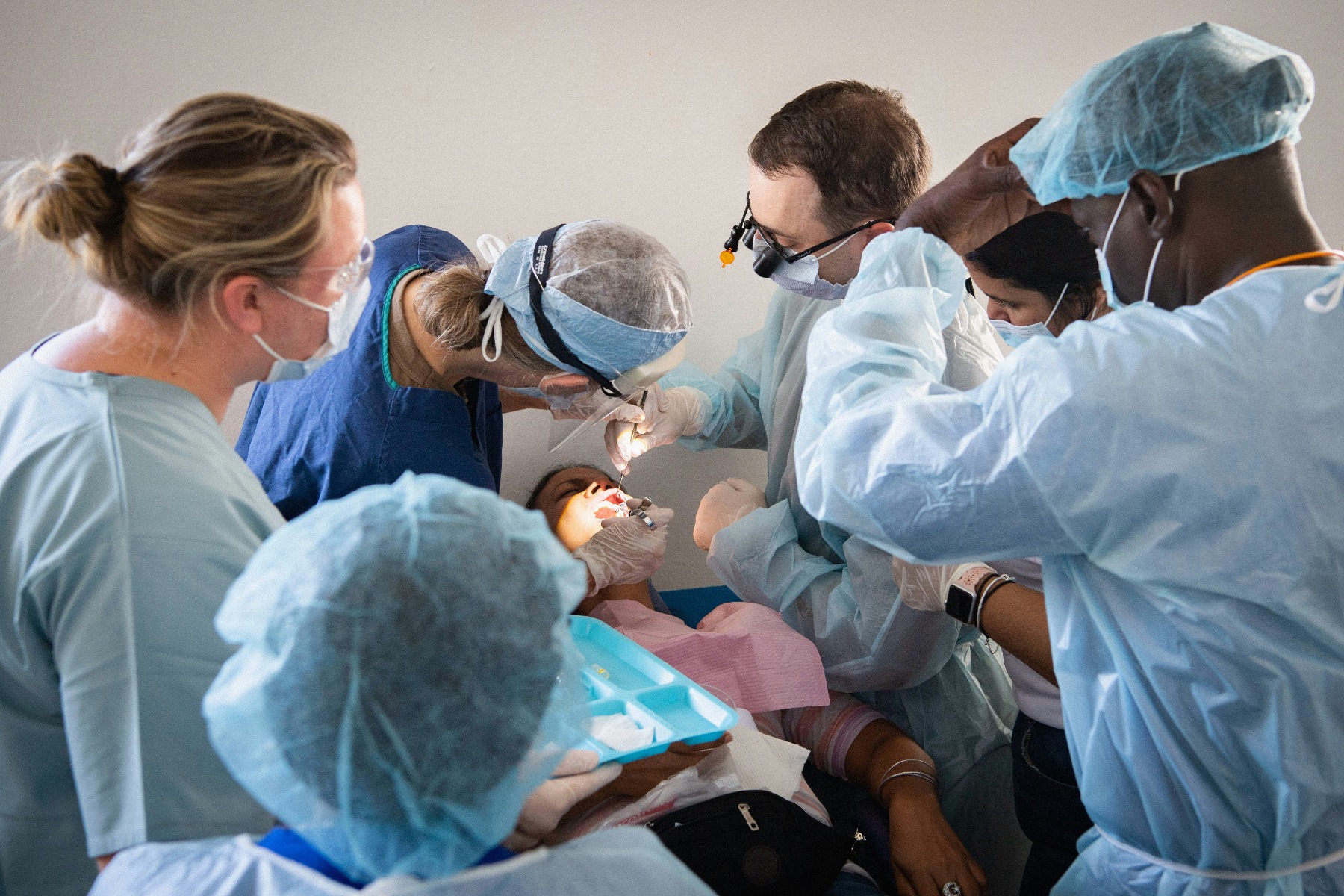
Classroom knowledge gets you through the door. Clinical hours build the muscle memory that keeps patients safe.
Accredited surgical technology programs combine didactic instruction (anatomy, microbiology, pharmacology, and surgical procedures) with substantial hands-on lab work and supervised clinical rotations in operating rooms. By the time a graduate finishes a program, they've scrubbed into procedures, managed live sterile fields, and worked alongside practicing surgical teams.
Certification through recognized credentialing bodies signals to employers that a candidate meets a vetted standard. The majority of surgical technologists (72%) work in hospital settings, where facility standards and credentialing requirements are typically the most rigorous. Outpatient surgery centers, physician offices, and specialty clinics make up the remainder of the employer landscape.
Want to Test Your Knowledge First?
Before committing to a program, it helps to know where you stand. Health Tech Academy offers a free practice exam so you can benchmark your current knowledge and see how the material feels.
Take Free Practice Exam →What Sets Surgical Technologists Apart from Other OR Roles
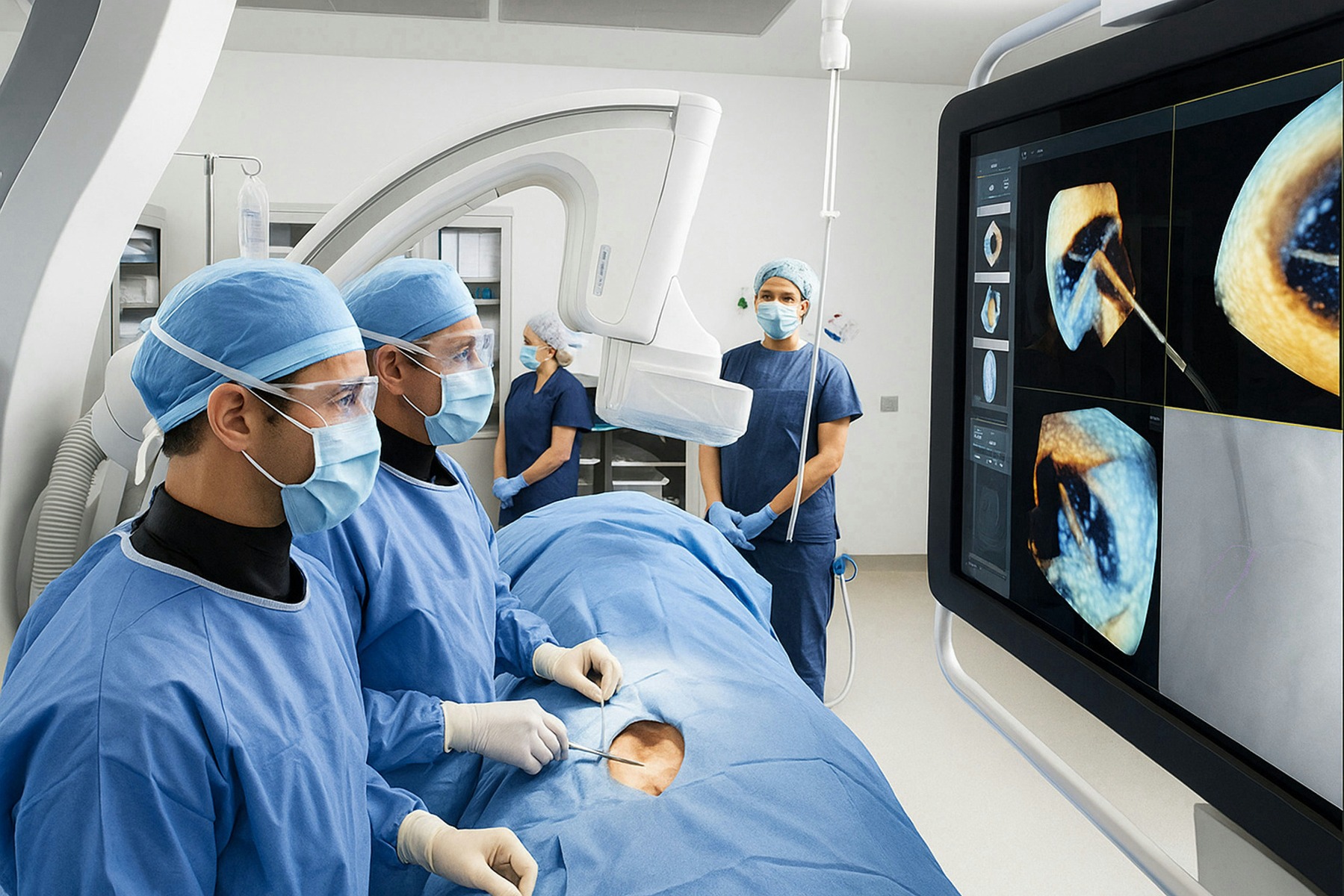
People frequently confuse surgical technologists with OR nurses, and while both are essential, they are not interchangeable.
"OR nurses can function in both the circulating role and the scrub role, but the surgical tech can only function in the scrub role. Their focus is on the technical and procedural aspects of the surgery and ensuring a safe and efficient surgical environment. While the surgical tech is the expert in the sterile field and instrument management, the OR nurse is the overall patient advocate and coordinator of care."
– Sonja Chambers, MSN, RN, CNOR, a Nursing Professional Development Specialist and Certified Surgical Technologist with 35 years of OR experience
Neither role subsumes the other. They are complementary – designed to cover different dimensions of patient safety during the same procedure.
Surgical technologists also differ from surgical assistants, who have additional training and may perform more hands-on tasks during procedures, such as retracting tissue, suturing, or closing incisions. The surgical technologist role is the foundational entry point, and the most direct path into the OR.
Preparation is Precision in Surgical Tech Roles
Surgical technology is a profession where preparation determines outcomes, and where the gap between a good tech and a great one shows up in the OR every single day. The pre-op readiness, the intra-op precision, the post-op accountability –each phase demands a distinct set of competencies that training builds and certification validates.
If you're weighing whether this career path fits, the best next step is an informed one.
Frequently Asked Questions and Answers
What Does a Surgical Technologist Do on a Daily Basis?
A surgical technologist prepares the operating room before surgery, sets up sterile instrument trays, counts all supplies with the circulating nurse, assists the surgeon intra-operatively by passing instruments and maintaining the sterile field, handles tissue specimens, and breaks down and restocks the room after each procedure. On a busy hospital shift, this cycle repeats multiple times.
Is a Surgical Technologist the Same as a Scrub Tech?
Yes. "Scrub tech," "scrub technologist," and "surgical technologist" are all terms for the same role. The name "scrub tech" comes from the surgical scrub – the hand and arm washing protocol performed before entering the sterile field.
How Long Does it Take to Become a Surgical Technologist?
Program lengths vary. Traditional associate degree programs typically take about two years. Accelerated and online certification programs can be completed in significantly less time – Health Tech Academy's program, for instance, runs 16 weeks and leads to the NRST credential through the AAH.
What Certification do Surgical Technologists Need?
The most widely recognized credential is the Certified Surgical Technologist (CST) designation, administered by the NBSTSA. The National Registry Surgical Technologist (NRST) credential through the AAH is another recognized certification pathway. Most states now require national certification, and many employers list it as a condition of hire.
What Skills are Most Important for a Surgical Technologist?
Technical precision, knowledge of surgical instrumentation, mastery of sterile technique, the ability to anticipate a surgeon's next move, and composure under pressure rank at the top. Strong communication skills and physical stamina – the ability to stand for several hours during long procedures – are equally important in day-to-day practice.
Where Do Surgical Technologists Work?
Most work in hospitals. Others are employed in outpatient surgery centers, physicians' offices, dental surgery facilities, and specialty clinics. Travel surgical technologist positions, which place credentialed techs in temporary assignments across the country, have grown substantially and often come with higher compensation.