The Sterile Processing Numbers Behind Productivity
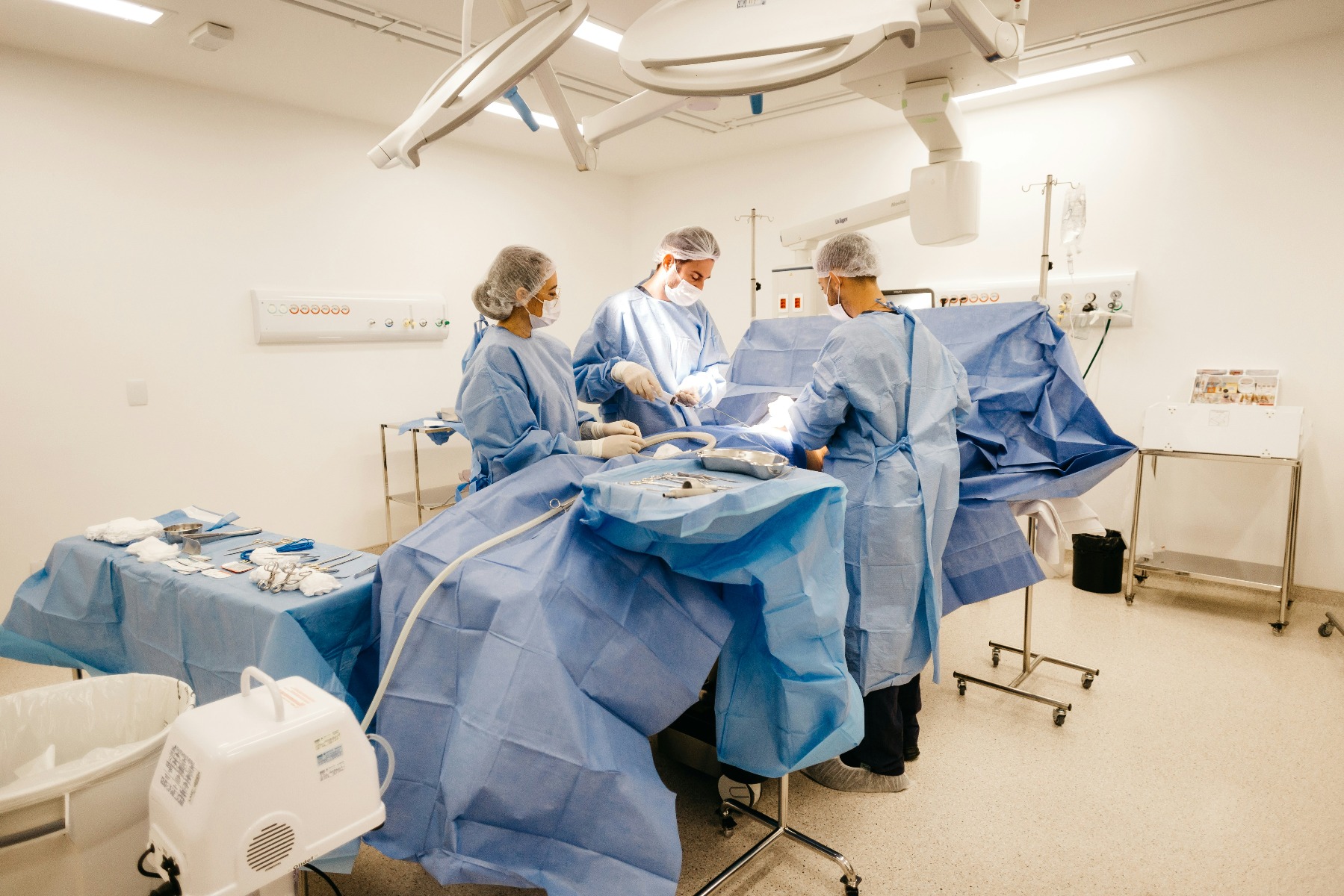
Sterile processing productivity is more layered than "how many trays did you turn over tonight." Department managers are tracking multiple data points simultaneously, and the ones that end up in your personnel file may not be what you expect.
According to Sullivan Healthcare Consulting, general industry benchmarks for Sterile Processing Department (SPD) technician output are 2–3 case carts processed through the decontamination room per hour, per person, and 3–4 trays assembled per hour in the assembly area – accounting for a mix of complex and minor instrument sets. For emergent cases, the expectation is that a case cart goes from identified to picked and ready in seven minutes. That last benchmark gets people. Seven minutes is not much runway.
Many facilities use an industry reference of approximately 24 minutes per instrument tray for the complete reprocessing cycle. That figure is drawn from data gathered by instrument tracking software companies operating across multiple health systems, and it's used by consultants and hospital administrators to justify or challenge staffing ratios.
OR time costs between $60 and $270 per minute, depending on the facility, surgeon, and staff in the room. That context makes the productivity expectations placed on SPD techs significantly less arbitrary than they appear on a shift report.
Tray turnaround time is widely considered the single most actionable sterile processing performance metric.
"Tray turnaround time – from a tray's arrival in the SPD through the full processing cycle to sterile storage – is arguably the most important data point to assist with instrument inventory planning and case scheduling. It connects directly to whether the OR runs on schedule, and by extension, to revenue, surgeon satisfaction, and patient outcomes."
– Ross Polston, National Manager of Planning & Design at Belimed
Unprocessed trays at 7 AM is another metric that catches technicians off guard. Many departments count how many trays from the previous surgical day remain unprocessed at the start of the morning. A high number doesn't automatically mean someone underperformed, but it triggers scrutiny. Leaders use it to assess volume-versus-staffing alignment and to pinpoint whether workflow bottlenecks concentrate on a specific shift.
Accuracy Benchmarks: The Metrics That Don't Forgive Sloppiness
Accuracy metrics carry more weight during patient safety audits and Joint Commission surveys. Getting through 20 trays per shift means nothing if two of them have missing instruments or compromised sterile barriers.
The widely cited benchmark for case cart error rate is 1% – no more than one error per 100 cases picked. Errors in this category include:
- Missing instruments not noted on the tray label.
- Wrong or broken instruments.
- Items with remaining bioburden.
- Missing chemical integrators.
- Mislabeled trays.
- Sets that weren't sterile when needed.
Incomplete tray and missing instrument rates are tracked individually at most facilities with instrument management systems. The expectation during audits is that the documentation trail is clean and that tray assembly reflects what's on the count sheet.
Biological indicator (BI) and chemical indicator (CI) compliance is another area where techs get caught during surveys. Every sterilization load must have appropriate chemical indicators, and biological monitoring must be conducted consistently per the facility's protocol and Association for the Advancement of Medical Instrumentation (AAMI) ST79 guidelines. A missing integrator on a tray gets flagged as both an accuracy error and a compliance gap – it shows up in two separate columns on an audit report.
Rejection rates and packaging failures round out the accuracy picture. Tears in wrapping, compromised seals, missing indicators, and event-related contamination discovered at the point of use are tracked and trended over time. A spike in rejection rates often triggers a root-cause analysis, and the assembled record of a tray is traceable in instrument tracking systems.
Compliance Benchmarks: What Accreditation Surveyors Monitor
If productivity and accuracy are what your manager tracks daily, compliance metrics are what the Joint Commission, Det Norske Veritas and Germanischer Lloyd (DNV GL), or Centers for Medicare & Medicaid Services (CMS) surveyors focus on when they walk through the door unannounced.
The compliance side of sterile processing performance metrics centers on adherence to established standards – primarily AAMI ST79, manufacturer instructions for use (IFUs), and facility-specific policies. Surveyors are looking for whether staff can demonstrate that they know and follow those standards.
"There are so many updated standards and practices that require sterile processing staff to be vigilant in having the most updated information and challenging their current processes to consistently improve their efforts and quality outcomes. It takes time to follow every step of an IFU for cleaning a medical device, but the time it takes to perform the cleaning tasks is severely underestimated by many facilities."
– Steven J Adams, RN, BA, CRCST, then-President of IAHCSMM (now HSPA) and RN Manager of Central Sterile Processing at Sinai Hospital in Baltimore
That underestimation is what surveyors probe. They'll ask technicians directly:
- Can you walk me through how you clean this specific scope?
- What does the IFU say about cycle parameters for this tray?
- Is your annual competency documentation current?
Staff certification and continuing education records are scrutinized during surveys. Many states now mandate Certified Registered Central Service Technician (CRCST) or equivalent certification for SPD technicians, and even where it isn't legislatively required, accreditation bodies and major health systems require it internally. A department where a significant share of techs lack current credentials is a compliance red flag.
Equipment maintenance and sterilizer load documentation are equally auditable. Every sterilization cycle must be logged, and biological indicator results – along with their incubation and release records – must be retained. Gaps in documentation get cited as compliance failures regardless of whether patient harm occurred.
Getting Certified Before the Audit Finds You Unprepared

The CRCST credential, offered through the Healthcare Sterile Processing Association (HSPA), is the most widely recognized entry-level certification in the field. It requires 400 hours of verified hands-on experience, a passing score of 70% or above on a 150-question exam, and annual renewal through continuing education.
Health Tech Academy's 16-week Sterile Processing Program prepares you specifically for the CRCST – covering the seven content domains assessed on the exam and building the foundational knowledge that auditors and employers expect to see demonstrated in practice.
Hear from One of Our Students
How Sterile Processing Performance Is Evaluated During Audits and Annual Reviews

Most SPD technicians assume their annual review is about attendance and attitude. That's part of it, but the data that influences raises, advancement, and continued employment is metric-driven.
Instrument tracking system data is now the center of individual performance evaluation at facilities that have implemented it. These systems log:
- Who assembled each tray.
- When it was assembled.
- Whether it passed inspection.
- How long the process took.
If a tray with bioburden is flagged at the point of use, the system generates a report that includes the technician's ID. That information goes directly into the incident record.
The AAMI benchmarking framework is used by many departments to establish worked-hours-per-unit (WHPU) standards – calculating how many staff-hours should be needed to process a given volume of work. When output doesn't align with those projections, it prompts a conversation. When it consistently falls short, it becomes a documented performance issue.
During Joint Commission or CMS surveys, evaluators often conduct direct staff interviews rather than reviewing binders. A technician who can articulate why they follow a specific cleaning protocol, cite the relevant standard, and demonstrate technique in real time is a direct reflection of the department's overall compliance posture. Departments that perform well in surveys invest in making sure all staff can speak to the "why" behind every step.
- Customer satisfaction surveys sent to OR teams and surgeons also feed into SPD performance reviews.
- These are scored and tracked over time.
- A pattern of complaints about incomplete sets, late trays, or instrument quality eventually reaches department leadership – and those complaints get correlated with shift logs and tray assembly records to identify where breakdowns occur.
One metric that rarely surfaces in workforce training is first case on-time starts (FCOTS). When the first surgical case of the day is delayed because instrumentation isn't ready, that delay is documented with a cause code. Repeated SPD-related FCOTS delays are a departmental performance issue discussed at the executive level.
Watch Our Podcast on Transforming the Healthcare Workforce Using AI
Sterile Processing Metrics That Can Define Your Professional Reputation
- Scope processing compliance rates: High-level disinfection (HLD) documentation for flexible endoscopes is among the most frequently cited areas of deficiency in surveys.
- Instrument repair cycle tracking: Instrument tracking systems flag when sets are overdue for refurbishment. Technicians who consistently identify damaged instruments during assembly contribute to a measurable reduction in deferred repairs.
- Shift-level backlog data: Most departments track the volume of unprocessed work at the start and end of each shift. A technician who consistently leaves less backlog for the incoming shift is contributing to an improvement in department flow – and that data is visible to supervisors with access to the tracking system.
What Certified Sterile Processing Technicians Should Prepare For
Certification is the difference between operating on instinct and operating on a documented, evidence-based framework that aligns with how your department is audited and evaluated.
Technicians who've completed structured CRCST preparation tend to process IFUs faster, document more accurately, and recognize compliance gaps before they become audit findings.
The CRCST pass rate was 75% in 2021 – meaning 1 in 4 test-takers didn't clear it on the first attempt. Preparation counts more than confidence here.
Try our free practice exam from Health Tech Academy to gauge your readiness before you register for the official CRCST.
Get Ahead of Performance Audits
Sterile processing performance metrics are specific, documented numbers that determine whether your department passes its next survey, whether patients are protected during every procedure, and whether your career moves forward or stalls at the next review cycle.
Knowing what's being measured – tray throughput, error rates, documentation compliance, sterilizer load records, and certification status – puts you ahead of most technicians who only learn this after they've already been through an audit.
Frequently Asked Questions and Answers
What are the Most Important Sterile Processing Performance Metrics for Technicians?
The most closely tracked metrics include tray assembly throughput (3–4 trays per hour in the assembly area), case cart error rate (benchmark: 1% or fewer errors per 100 cases), tray turnaround time, biological and chemical indicator compliance, and documentation accuracy. At facilities with instrument tracking systems, individual technician data is logged in real time.
How is Sterile Processing Technician Performance Measured During a Joint Commission Survey?
Surveyors assess compliance with AAMI standards and IFUs, review sterilizer load and biological indicator documentation, evaluate equipment maintenance records, and conduct direct staff interviews to confirm that technicians understand and can articulate the protocols they follow. Certification records and continuing education documentation are also reviewed.
Does CRCST Certification Affect How Employers Evaluate Performance?
Yes. Data from departments using instrument tracking systems shows measurable differences in quality and productivity between certified and uncertified technicians. Many health systems now require certification for all SPD staff, and it is a prerequisite for advancement into lead technician or supervisory roles at most major facilities.
What is the Case Cart Error Rate Benchmark in Sterile Processing?
The industry benchmark is 1% – no more than one error per 100 cases picked. Errors include missing instruments, wrong or broken instruments, items with bioburden, missing chemical integrators, and mislabeled or non-sterile trays.
What is WHPU and Why Does it Matter for Sterile Processing Technicians?
WHPU stands for worked hours per unit – a metric used to calculate how many staff-hours should be required to process a given volume of instrumentation. It's used by department leaders and administrators to evaluate staffing efficiency and identify whether individual output aligns with departmental benchmarks. The industry reference is approximately 24 minutes per instrument tray for the complete reprocessing cycle.
How Often are Sterile Processing Technicians Evaluated on Performance Metrics?
Formal annual reviews typically incorporate instrument tracking data, documentation compliance rates, and supervisor observation. However, metric data is generated continuously by tracking systems, so output is visible to department leadership at any time. Accreditation surveys can occur unannounced and often include direct evaluation of individual technician knowledge and technique.



